Overview of Wound Care Assessment
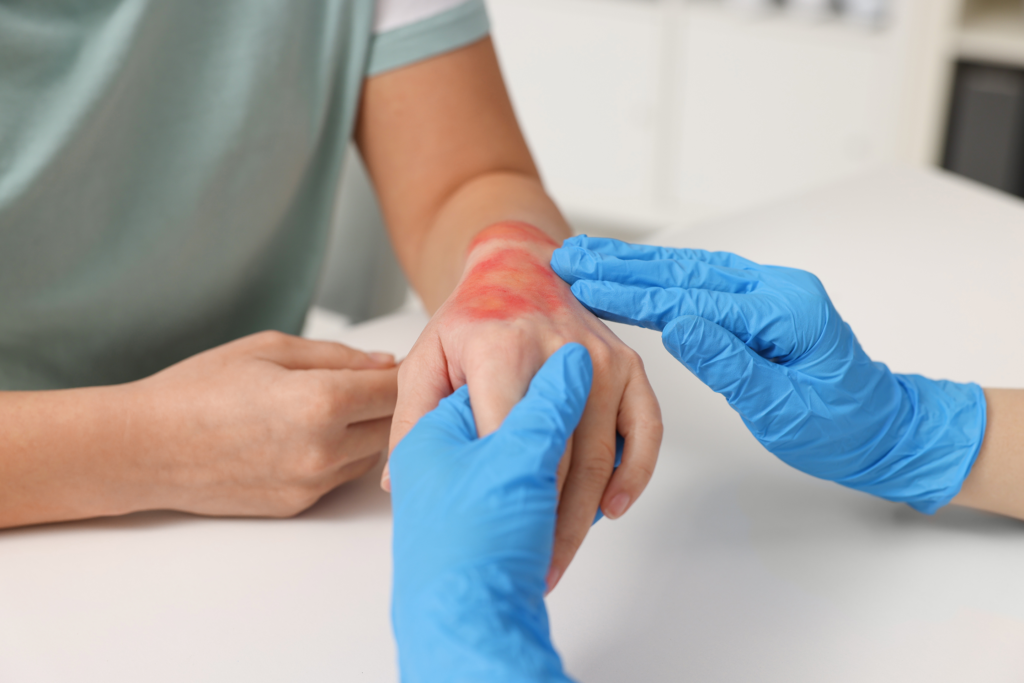
Wound care assessment is a structured clinical process used to evaluate the condition of a wound and guide appropriate treatment decisions. It plays a critical role in determining how well a wound is healing and whether complications are developing. Healthcare professionals rely on wound care assessment to establish baseline measurements and track changes over time. This process applies to acute injuries, surgical wounds, and chronic conditions that require long-term management. Proper evaluation helps reduce risks such as infection, delayed healing, and tissue deterioration. It also supports individualized treatment planning based on patient needs and wound characteristics. In modern healthcare, wound care assessment is considered an essential skill for nurses, physicians, and wound care specialists. Accurate assessment improves communication across care teams and enhances patient outcomes.
Wound care assessment involves both visual inspection and clinical judgment supported by standardized tools. It is not a one-time task but an ongoing process that evolves with the wound’s healing progress. Clinicians must consider both local wound conditions and systemic health factors. A thorough approach ensures that underlying causes are addressed, not just surface symptoms. This makes wound care assessment a foundation for effective wound management in clinical practice.
Types of Wounds Commonly Encountered in Clinical Practice
Wounds vary widely depending on their origin, severity, and healing capacity. Understanding wound categories is essential for proper wound care assessment and treatment planning. Acute wounds typically result from trauma, burns, or surgical procedures and usually follow a predictable healing path. Chronic wounds, on the other hand, persist for extended periods due to underlying health conditions such as diabetes or poor circulation. These wounds often require long-term monitoring and specialized care strategies.
In clinical settings, infected wounds present additional challenges due to bacterial contamination and inflammation. These wounds require close observation during wound care assessment to prevent systemic complications. Post-operative wounds also require regular evaluation to ensure proper healing and to detect early signs of complications. Pressure injuries are another common category, especially among immobile patients, and require staging and ongoing monitoring. Each wound type demands a tailored approach during evaluation.
Healthcare providers must also consider mixed-type wounds that present characteristics of more than one category. These cases require careful differentiation during wound care assessment to avoid mismanagement. Understanding wound classification helps clinicians select appropriate dressing materials and treatment methods. It also supports more accurate prognosis and healing expectations. Recognizing wound types is a foundational step in clinical evaluation.
Core Components of Wound Care Assessment
Wound care assessment involves multiple clinical observations that provide a complete picture of wound status. These components help clinicians understand healing progress and identify potential complications early. One of the most important aspects is measuring the wound’s size, including length, width, and depth. Tissue composition within the wound bed is also evaluated to determine healing activity. The presence of granulation tissue, slough, or necrotic tissue provides important diagnostic information. Exudate characteristics such as amount, color, and odor are also carefully assessed.
Pain levels reported by the patient contribute valuable insight into wound condition. Surrounding skin integrity is examined for signs of irritation, maceration, or infection spread. Circulation and perfusion status are also considered, especially in chronic wound cases. These combined factors form the basis of effective wound care assessment.
Key elements commonly evaluated include:
- Wound size and dimensional changes over time
- Tissue type present in the wound bed
- Exudate amount, color, and odor characteristics
- Presence of infection indicators such as redness or warmth
- Condition of surrounding skin and tissue
- Patient-reported pain and discomfort levels
- Blood flow and oxygenation to the affected area
Each of these elements contributes to a comprehensive understanding of wound status. Careful documentation of these findings ensures consistency in monitoring and treatment planning. Small changes in any of these components can indicate significant shifts in healing progression.
Step-by-Step Clinical Wound Assessment Process
The wound care assessment process follows a structured sequence to ensure accuracy and consistency. It begins with reviewing the patient’s medical history and identifying underlying conditions that may affect healing. Conditions such as diabetes, vascular disease, or immune disorders are especially important. The next step involves visual inspection of the wound and surrounding area. Clinicians observe color, tissue condition, and any visible signs of infection or trauma.
Measurement of the wound is performed using standardized tools to ensure consistency. Documentation is completed immediately to avoid errors or omissions. Photographic records may also be used for comparison over time. Reassessment is scheduled regularly depending on wound severity and clinical judgment.
During each visit, clinicians compare current findings with previous wound care assessment records. This allows them to identify trends in healing or deterioration. Adjustments to treatment plans are made based on these observations. Communication with the healthcare team ensures coordinated care. This structured process supports safe and effective wound management.
Tools and Technologies Used in Wound Care Assessment
Modern wound care assessment relies on both traditional tools and advanced technologies. Simple measurement tools such as rulers and probes are still widely used in clinical settings. These tools help determine wound dimensions accurately and consistently. Digital photography has become an essential part of documentation and monitoring. It allows clinicians to track visual changes over time with greater precision.
Electronic health records support structured documentation and interdisciplinary communication. Some healthcare facilities use digital wound imaging systems for enhanced analysis. These systems can measure wound size automatically and detect subtle changes. Advanced technologies may also assess tissue oxygenation and blood flow. Such innovations improve the accuracy of wound care assessment.
Telemedicine platforms are increasingly used for remote wound monitoring. Patients can submit images for evaluation, reducing the need for frequent in-person visits. This approach is especially useful for chronic wound management. Technology continues to enhance efficiency and accuracy in wound assessment. However, clinical judgment remains essential in interpreting all data.
Identifying Infection and Complications During Assessment
Detecting infection early is one of the most important goals of wound care assessment. Local signs of infection include redness, warmth, swelling, and increased pain. Discharge with foul odor or unusual color may also indicate bacterial activity. Systemic signs such as fever or fatigue suggest more serious complications. Differentiating between colonization and active infection is essential for proper treatment.
Unmanaged infection can significantly delay healing and lead to tissue damage. In severe cases, it may result in systemic illness requiring urgent intervention. Clinicians must remain vigilant during every wound care assessment. Early detection allows for timely treatment and improved outcomes. Antibiotic use should be carefully managed to prevent resistance.
Wound Healing Phases and Their Clinical Implications
Wound healing occurs in distinct biological phases that guide clinical evaluation. The hemostasis phase involves initial clot formation to stop bleeding. The inflammatory phase follows, where the body removes debris and fights infection. During the proliferative phase, new tissue begins to form and fill the wound bed. The maturation phase strengthens newly formed tissue over time.
Each phase presents specific characteristics that influence wound care assessment. Recognizing these stages helps clinicians determine whether healing is progressing normally. Deviations from expected patterns may indicate complications. Understanding healing phases also supports treatment selection. This knowledge is essential for accurate clinical decision-making.
Documentation Standards in Wound Care Assessment
Accurate documentation is a critical part of wound care assessment. It ensures continuity of care and supports clinical decision-making. Records must include detailed descriptions of wound size, appearance, and changes over time. Consistent terminology helps avoid confusion among healthcare providers. Standardized forms and charts are often used for uniform reporting.
Proper documentation also has legal and regulatory importance. It provides evidence of care provided and supports treatment justification. Incomplete records can lead to miscommunication and treatment errors. Clear documentation improves collaboration among multidisciplinary teams. It also enhances patient safety and care quality.
Patient Factors Influencing Wound Healing
Several patient-related factors significantly impact wound healing outcomes. Chronic conditions such as diabetes can slow the healing process. Poor nutrition reduces the body’s ability to repair tissue effectively. Aging skin is more fragile and prone to injury. Smoking reduces oxygen supply to tissues, delaying recovery.
Medications may also influence healing speed and immune response. Hydration status plays a role in maintaining healthy tissue function. Psychological stress can indirectly affect immune performance. Each of these factors is considered during wound care assessment. Addressing underlying issues improves healing potential.
Special Considerations in Complex Wound Assessment
Complex wounds require more detailed evaluation and specialized care. Pressure injuries require staging based on tissue damage severity. Arterial and venous wounds differ in appearance and treatment approach. Immunocompromised patients may show atypical healing responses. Pediatric and elderly patients require age-specific assessment techniques.
Post-surgical wounds must be monitored for dehiscence or infection. These cases often require more frequent wound care assessment. Complex wounds may also involve multiple contributing conditions. Care plans must be adjusted based on ongoing evaluation. Specialized expertise improves outcomes in these cases.
Challenges in Accurate Wound Care Assessment
Wound care assessment can be challenging due to variability in clinical practice. Subjective interpretation of wound characteristics may lead to inconsistencies. Limited resources can restrict access to advanced diagnostic tools. Patient non-compliance can affect monitoring accuracy. Complex wounds often require long-term evaluation and adjustment.
Differences in training among healthcare providers may also affect consistency. Environmental factors in clinical settings can influence assessment quality. Time constraints may limit detailed evaluation in busy facilities. Despite these challenges, standardized protocols help improve accuracy. Continuous training supports better clinical performance.
Evidence-Based Practices in Wound Care Assessment
Evidence-based practice plays a central role in wound care assessment. Clinical guidelines provide standardized approaches to evaluation and treatment. Regular reassessment ensures that care plans remain effective. Multidisciplinary collaboration enhances decision-making quality. Research findings help refine assessment techniques and improve outcomes.
Best practices emphasize consistency and accuracy in evaluation. Updated protocols reflect advances in wound care science. Continuous education supports professional development. Evidence-based methods reduce variability in clinical practice. This leads to improved patient outcomes and safety.
Communication and Patient Education in Wound Management
Effective communication is essential in wound care assessment. Patients must understand their condition and treatment plan clearly. Educating patients improves adherence to care instructions. Home care guidance helps prevent complications. Recognizing warning signs allows early intervention.
Clear communication builds trust between patients and healthcare providers. It also encourages active participation in healing. Patients who understand wound care are more likely to follow recommendations. Education improves long-term outcomes and reduces recurrence. This makes communication a vital part of clinical practice.
Multidisciplinary Approach to Wound Care Assessment
Wound care assessment benefits greatly from a team-based approach. Nurses often perform initial evaluations and ongoing monitoring. Physicians provide medical oversight and treatment planning. Specialists contribute expertise in complex cases. Nutritionists support healing through dietary planning.
Physical therapists assist with mobility and pressure reduction strategies. Collaboration ensures comprehensive care planning. Communication between team members improves efficiency. Shared decision-making enhances patient outcomes. Multidisciplinary care strengthens overall wound management systems.
Takeaway
Wound care assessment is a structured and essential process in healthcare that supports accurate evaluation and effective treatment planning. It requires consistent observation, documentation, and clinical judgment to ensure proper healing progress. Each assessment provides valuable insight into wound condition and potential complications. Patient health status and underlying conditions significantly influence outcomes. A multidisciplinary approach enhances care quality and improves recovery results. Continuous monitoring allows timely adjustments to treatment strategies. Clear communication and education strengthen patient involvement in healing. Accurate wound care assessment remains a cornerstone of safe and effective clinical practice.