Pressure ulcers, also known as bedsores or decubitus ulcers, are injuries to the skin and underlying tissue caused by prolonged pressure. They often develop on areas of the body where bone and skin are in close contact, such as the heels, hips, and lower back. These wounds can affect anyone who is bedridden, immobile, or recovering from surgery, and without proper care, they can lead to serious complications, including infections, chronic pain, and reduced quality of life. Proper Pressure Ulcer Management is essential for preventing these outcomes, supporting healing, and improving the overall well-being of patients.
Early detection and treatment play a critical role in Pressure Ulcer Management. Bedsores can form quickly, sometimes within hours of sustained pressure, so recognizing early signs such as redness, swelling, or skin discoloration is vital. Pressure Ulcer Management not only addresses the wound itself but also considers the patient’s overall health, nutrition, mobility, and living environment, creating a comprehensive plan that promotes faster healing and prevents recurrence.
Signs and Stages of Pressure Ulcers
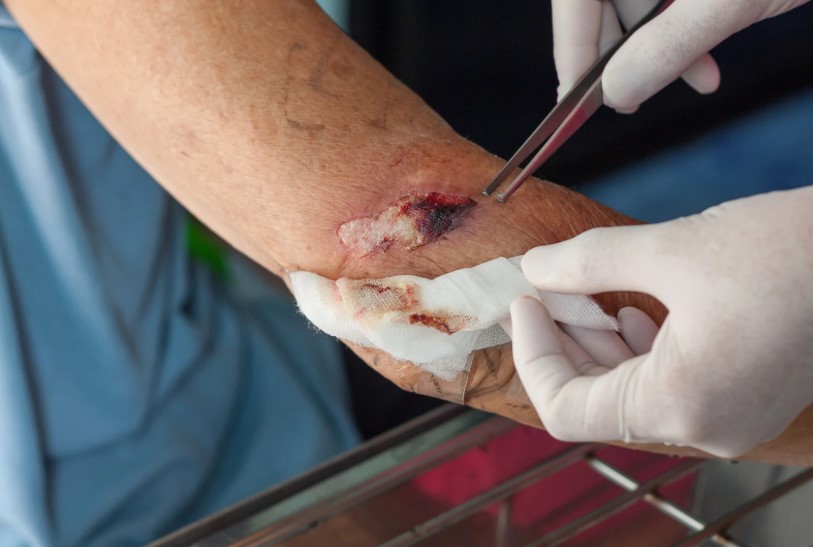
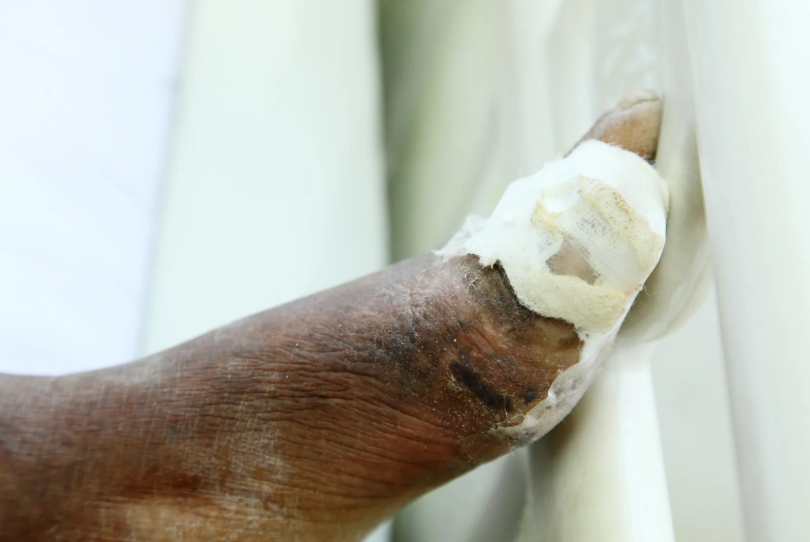
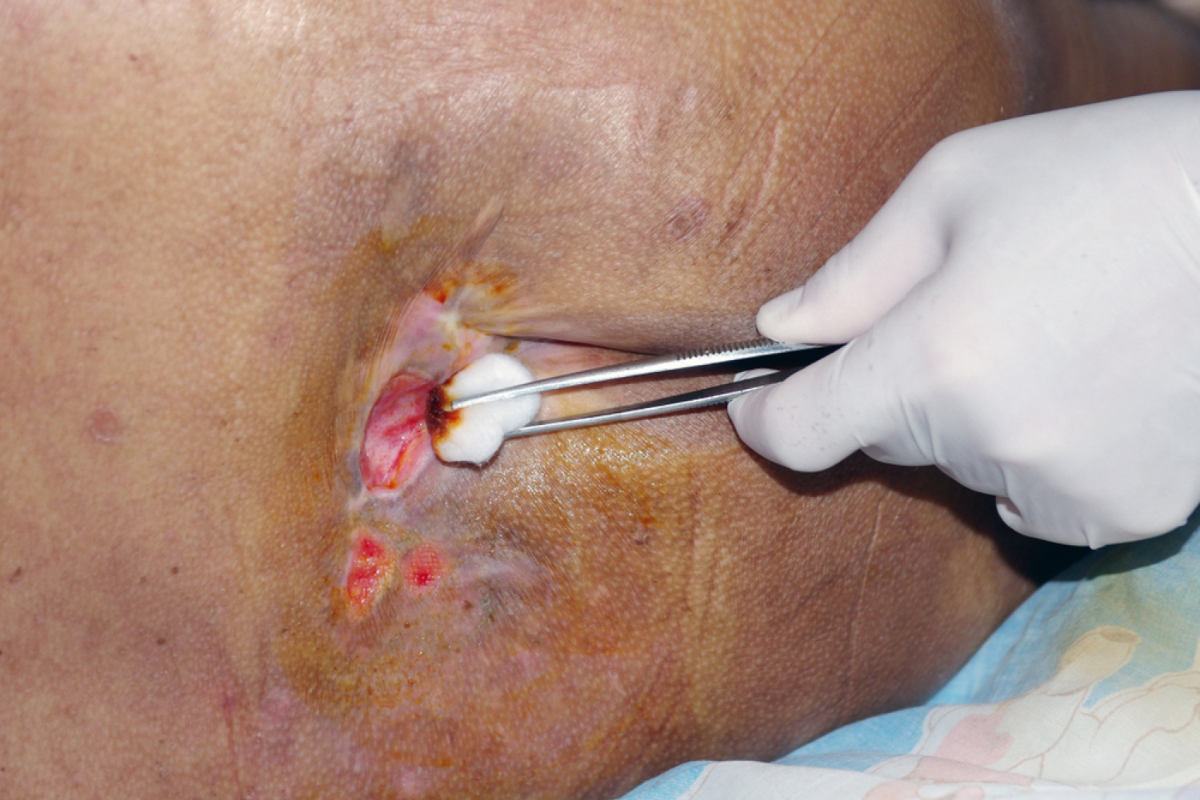
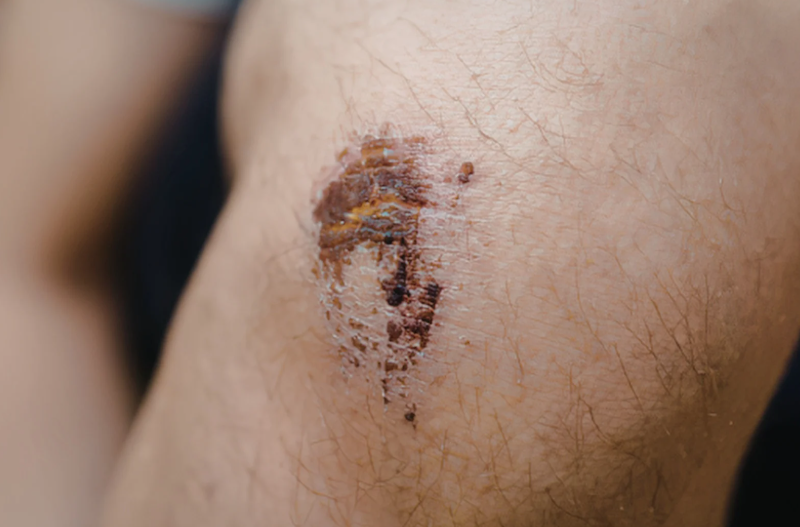
Understanding the stages of pressure ulcers is a cornerstone of effective Pressure Ulcer Management. These wounds are categorized into four stages, each indicating the severity of tissue damage. Stage 1 pressure ulcers appear as reddened skin that does not blanch when pressed. Stage 2 involves partial-thickness skin loss, presenting as an open sore or blister. Stage 3 pressure ulcers extend into the fat layer beneath the skin, forming deeper wounds. Stage 4 represents full-thickness tissue loss, potentially exposing muscles, tendons, or bone.
Recognizing these stages helps caregivers and healthcare professionals design targeted Pressure Ulcer Management plans. Early intervention during Stage 1 and Stage 2 can prevent progression, while Stage 3 and Stage 4 wounds require specialized treatment to manage infections, promote tissue regeneration, and reduce complications. Regular monitoring, repositioning, and proper skin care are critical practices that support Pressure Ulcer Management at every stage.
Why Specialized Pressure Ulcer Management Matters
Effective Pressure Ulcer Management is more than dressing a wound. Without proper care, pressure ulcers can worsen, leading to infections, chronic non-healing wounds, and even life-threatening complications. Standard home care may not provide the advanced assessment, debridement techniques, or wound therapies needed to achieve lasting recovery. Specialized Pressure Ulcer Management ensures that each patient receives a treatment plan tailored to the severity of the wound, underlying health conditions, and personal circumstances.
KALINGAP Wound Care Clinic in Quezon City and Metro Manila provides professional Pressure Ulcer Management guided by experienced clinicians. Under the leadership of Dr. Lou Mervyn Tec, board-certified orthopedic surgeon and wound care specialist, the clinic delivers personalized care that integrates advanced medical technology with compassionate, patient-centered practices. The clinic’s approach ensures that every patient receives not only physical treatment but also education, preventive strategies, and emotional support, creating a holistic model of Pressure Ulcer Management.
Treatment Options at KALINGAP Wound Care Clinic
KALINGAP Wound Care Clinic offers a wide range of treatments designed to address pressure ulcers effectively and safely.
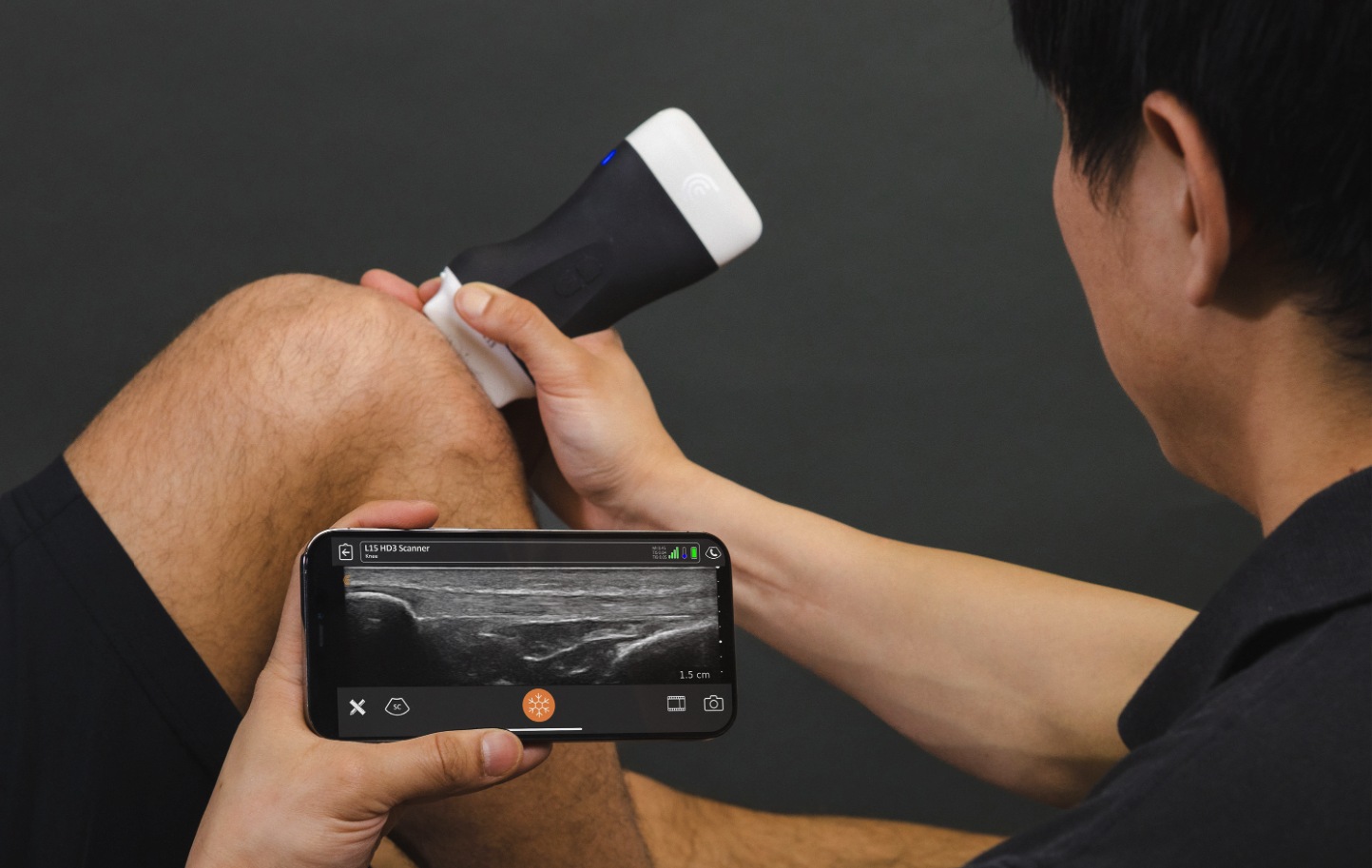
Advanced Wound Assessment is the first step in Pressure Ulcer Management. Each wound is carefully evaluated using evidence-based tools to determine its stage, depth, and risk factors. This assessment guides the development of a tailored treatment plan that prioritizes both wound healing and patient comfort.
Ultrasonic Debridement is another key service in Pressure Ulcer Management. This technique gently removes dead tissue without damaging healthy skin, promoting faster healing and reducing the risk of infection. Ultrasonic-assisted debridement is particularly beneficial for patients with sensitive or chronic wounds that require careful handling.
Negative Pressure Wound Therapy (NPWT) is a highly effective treatment for deep or persistent bedsores. This vacuum-assisted therapy enhances blood circulation, reduces swelling, and accelerates tissue regeneration. NPWT is often used alongside other Pressure Ulcer Management strategies to improve outcomes and shorten healing time.
Customized care plans form the foundation of comprehensive Pressure Ulcer Management. Patients receive advanced dressings, support surfaces, and offloading strategies tailored to their specific needs. These interventions help relieve pressure on affected areas, protect the skin, and prevent new ulcers from forming.
Infection Control and Management is crucial in Pressure Ulcer Management, as infected wounds can delay healing and increase the risk of serious complications. The clinic provides timely identification and treatment of infections, using antibiotics when necessary and monitoring healing progress closely.
Education and Prevention Programs empower both patients and caregivers to participate actively in Pressure Ulcer Management. Training sessions cover proper hygiene, nutritional guidance, repositioning techniques, and strategies to reduce pressure on vulnerable areas. These programs ensure that preventive measures are incorporated into daily routines, minimizing the risk of new ulcers.
Chronic Wound Management addresses long-term challenges associated with persistent pressure ulcers. Patients receive ongoing support to manage skin integrity, improve mobility, and maintain overall health, ensuring that Pressure Ulcer Management extends beyond the initial treatment period.
Preventing Pressure Ulcers: Tips for Caregivers and Patients
Preventive care is a critical component of Pressure Ulcer Management. Regular repositioning of bedridden patients reduces prolonged pressure on bony areas, decreasing the likelihood of ulcer formation. Support surfaces, such as specialized mattresses and cushions, also play an essential role in distributing weight evenly and relieving pressure points.
Maintaining proper hygiene and skin care is another cornerstone of effective Pressure Ulcer Management. Cleaning and moisturizing the skin regularly prevents dryness, cracking, and irritation that could contribute to wound development.
Nutrition and hydration are equally important. A well-balanced diet rich in protein, vitamins, and minerals supports tissue repair and overall immune function, enhancing the body’s ability to heal pressure ulcers.
Caregivers should also monitor patients for early signs of pressure ulcers, such as redness, warmth, or skin breakdown. Early detection allows prompt intervention, which is a key principle of successful Pressure Ulcer Management.
Why Choose KALINGAP Wound Care Clinic
KALINGAP Wound Care Clinic offers Pressure Ulcer Management services that combine medical expertise with a compassionate, patient-focused approach. Dr. Lou Mervyn Tec leads a team of trained professionals dedicated to providing advanced care tailored to each patient’s needs.
The clinic’s philosophy emphasizes Filipino values of kalinga (care) and lingap (nurture), ensuring that patients receive treatment in a supportive and understanding environment. KALINGAP addresses financial and accessibility challenges by offering affordable care options, community outreach programs, and educational resources, making Pressure Ulcer Management accessible to a wider population.
Patients benefit from comprehensive support that goes beyond wound care. Education, preventive guidance, emotional support, and long-term follow-up are integrated into every treatment plan, creating a seamless healing experience.
Patient Stories and Success Cases
Many patients have experienced remarkable recovery through KALINGAP’s Pressure Ulcer Management program. For instance, bedridden individuals with Stage 3 or Stage 4 ulcers have achieved significant healing using a combination of NPWT, ultrasonic debridement, and personalized care plans. Caregivers report that patient education sessions helped them maintain proper preventive care at home, reducing the likelihood of new ulcers. These success stories demonstrate the effectiveness of combining medical expertise with compassionate support, a hallmark of KALINGAP’s approach to Pressure Ulcer Management.
Frequently Asked Questions (FAQ)
What is Pressure Ulcer Management?
Pressure Ulcer Management is the process of assessing, treating, and preventing bedsores. It includes wound evaluation, dressing, infection control, advanced therapies, and preventive education.
How quickly can pressure ulcers develop?
Pressure ulcers can develop within hours of sustained pressure, especially on bony areas. Early detection and proper care are essential to prevent worsening.
Can pressure ulcers be completely healed?
Yes, with proper Pressure Ulcer Management, including advanced therapies, regular monitoring, and preventive care, most ulcers can heal completely.
Who should seek professional Pressure Ulcer Management?
Patients who are bedridden, immobile, recovering from surgery, or experiencing chronic wounds should seek professional care to prevent complications and promote healing.
What makes KALINGAP Wound Care Clinic different?
KALINGAP combines medical expertise, advanced treatment techniques, and a compassionate approach. The clinic also provides patient education, preventive care, and affordable services in Quezon City and Metro Manila.
How can caregivers prevent pressure ulcers at home?
Regular repositioning, proper hygiene, use of support surfaces, adequate nutrition, and monitoring for early skin changes are key preventive measures. Education programs from KALINGAP provide detailed guidance for caregivers.
Is Pressure Ulcer Management expensive?
KALINGAP offers affordable care options and community programs to make professional Pressure Ulcer Management accessible for a wider population.