Understanding the Medical Scope of Sever Wound Surgery
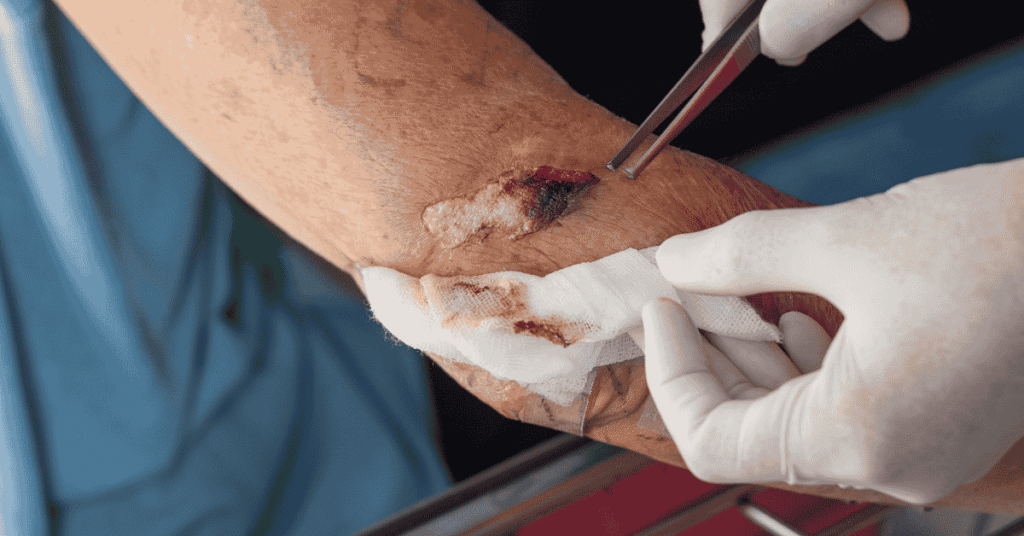
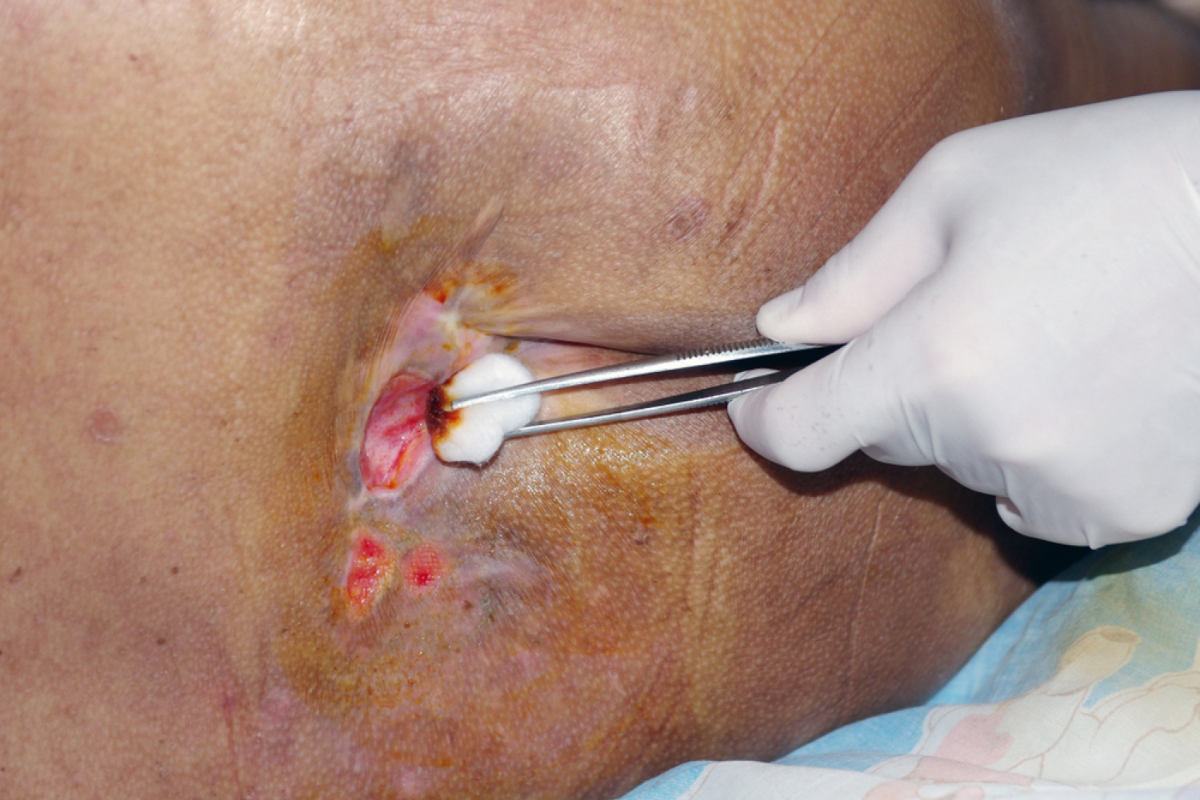
Sever wound surgery refers to specialized surgical intervention used to treat deep, traumatic injuries that involve extensive damage to skin, muscles, blood vessels, nerves, and sometimes bone structures. These injuries typically occur in high-impact situations such as vehicle collisions, industrial accidents, severe falls, or penetrating trauma. The complexity of these wounds requires immediate and highly coordinated medical care to prevent life-threatening complications. Without timely surgical intervention, patients face risks such as massive blood loss, infection, and permanent tissue damage. The primary goal of sever wound surgery is to stabilize the patient while restoring structural integrity and preserving as much function as possible. Medical teams often treat these cases as emergencies due to the rapid progression of complications. Every decision in the treatment process is guided by the extent of trauma and the patient’s overall stability.
Types of Injuries That Require Sever Wound Surgery
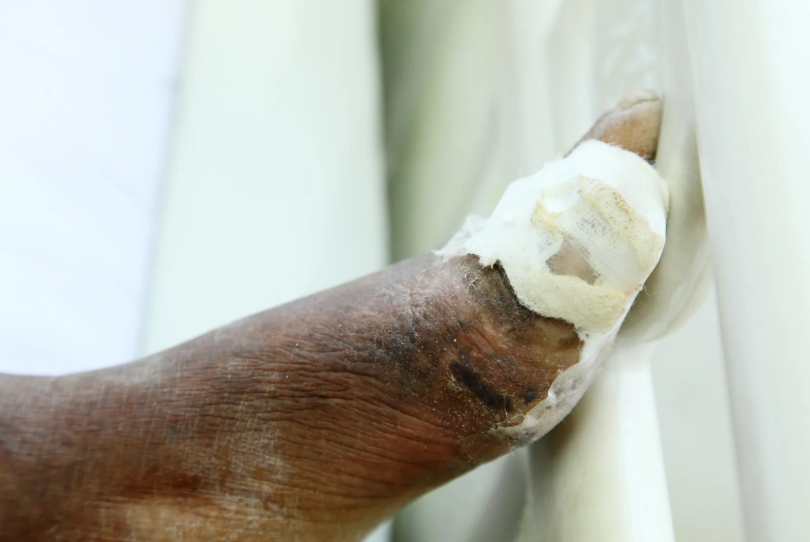
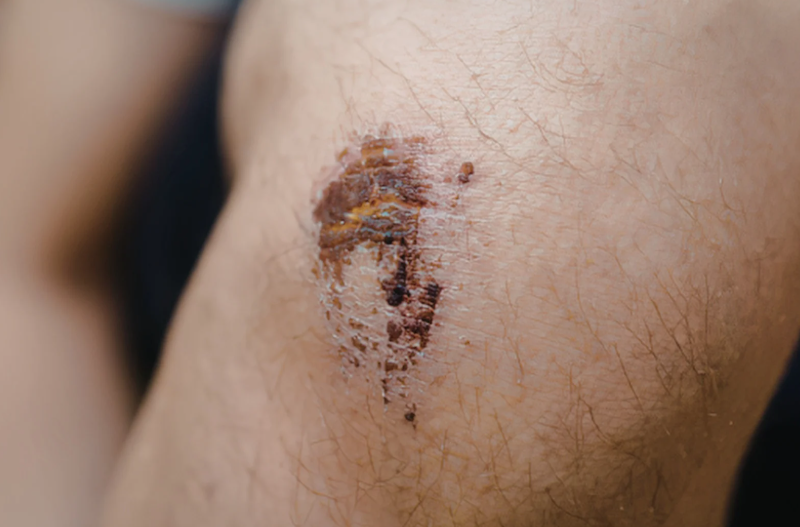
Different categories of injuries may require sever wound surgery, depending on depth and tissue involvement. Deep lacerations are among the most common and often involve significant bleeding and tissue separation. Crush injuries occur when prolonged force damages soft tissue and restricts blood flow, leading to possible necrosis. Avulsion injuries, where tissue is forcibly detached from the body, are particularly complex and require reconstructive procedures. Puncture wounds that penetrate deep into the body can damage internal organs and blood vessels, requiring immediate surgical exploration. Contaminated wounds with foreign materials such as metal, dirt, or glass increase infection risk significantly. Amputation-related injuries may involve partial or complete loss of limbs and require reconstructive or prosthetic planning. Each type demands a unique surgical approach tailored to the severity and location of injury.
Emergency Stabilization Prior to Sever Wound Surgery
Before performing sever wound surgery, emergency stabilization is critical to improve survival outcomes. The first priority is controlling bleeding using pressure dressings or tourniquets when necessary. Airway, breathing, and circulation are assessed immediately to determine patient stability. Immobilizing the injured area prevents further tissue damage during transport. Emergency responders must avoid contaminating the wound while providing care. Pain management may be initiated in controlled settings to reduce patient distress. Rapid transport to a trauma-equipped facility ensures surgical teams can act quickly. These early interventions significantly influence the success rate of sever wound surgery.
Diagnostic Process Before Sever Wound Surgery
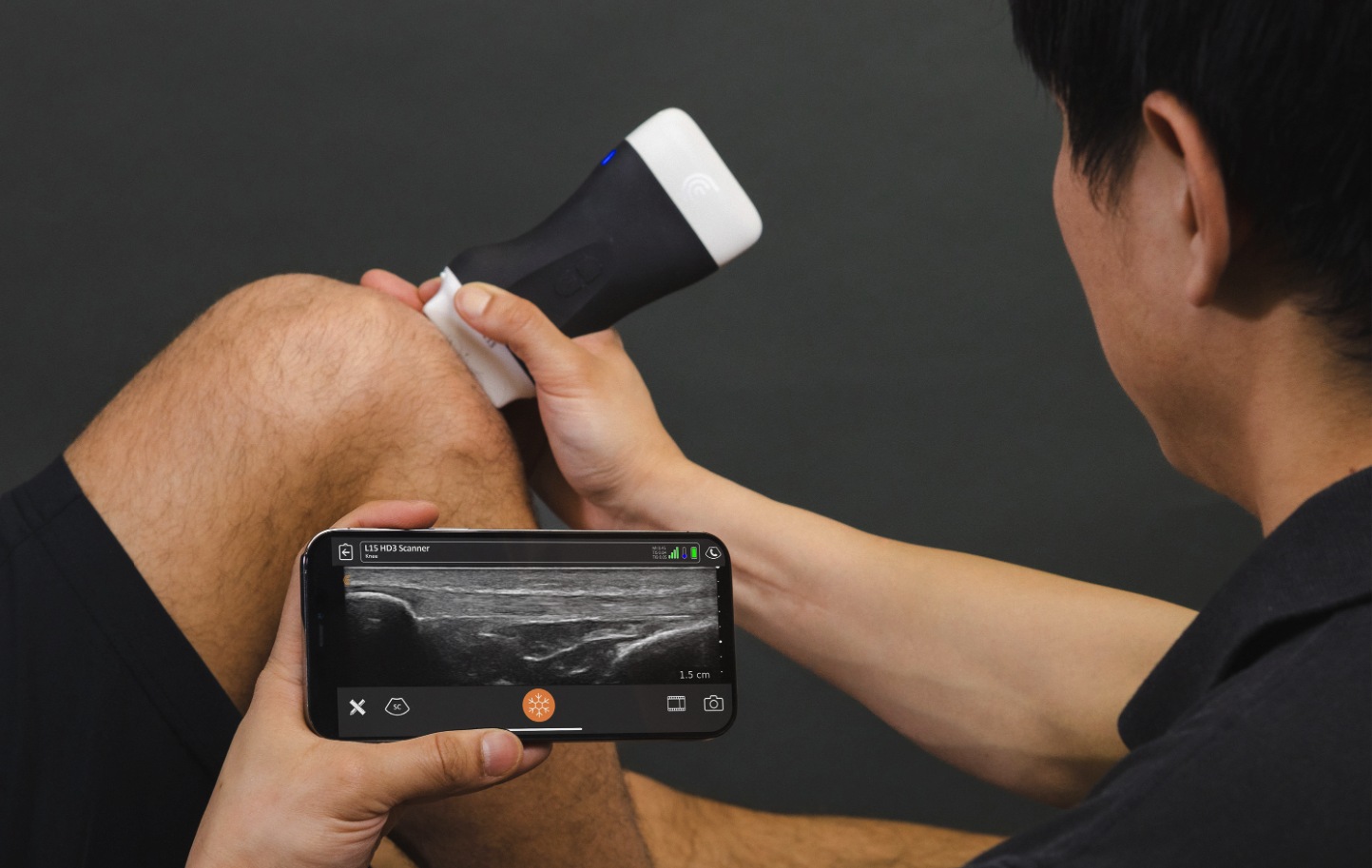
Accurate diagnosis is essential before proceeding with sever wound surgery, as it guides surgical planning. A physical examination is performed to assess visible injuries and identify potential hidden damage. Imaging tests such as X-rays help detect fractures or foreign objects inside the wound. CT scans provide detailed cross-sectional images for complex trauma evaluation. MRI scans are useful in assessing soft tissue, nerve, and ligament damage. Blood tests help identify infection markers and evaluate blood loss severity. Vascular assessments determine whether blood flow has been compromised in affected areas. These diagnostic tools allow surgeons to develop a precise and effective treatment strategy.
Surgical Procedures Involved in Sever Wound Surgery
Sever wound surgery involves multiple specialized techniques depending on injury severity. Debridement is performed to remove dead or infected tissue, reducing the risk of complications. Hemostasis techniques are used to stop active bleeding and stabilize the surgical field. Wound closure may be immediate or delayed depending on contamination levels. Skin grafting is often required when large tissue areas are lost. Reconstructive microsurgery allows surgeons to repair nerves and blood vessels with precision. Sutures, staples, or adhesives may be used to close wound edges effectively. Vacuum-assisted closure systems may also be applied to promote faster healing and fluid drainage.
Reconstructive Approaches in Severe Wound Treatment
Reconstruction plays a vital role in sever wound surgery, especially for extensive injuries. The primary goal is to restore both function and appearance of the affected area. Tissue grafts may be taken from other parts of the body to replace damaged skin. Bone reconstruction is sometimes necessary in cases involving fractures or structural damage. Surgeons may use flap techniques to transfer tissue with its blood supply intact. In extreme cases, prosthetic solutions are considered when natural repair is not possible. Reconstructive planning is often long-term and may require multiple surgeries. The success of reconstruction significantly impacts the patient’s mobility and quality of life.
Infection Prevention and Control in Sever Wound Surgery
Infection control is a major concern during sever wound surgery due to open tissue exposure. Surgical environments are maintained under strict sterile conditions to minimize contamination. Antibiotics are administered before and after surgery to reduce infection risk. Wound irrigation is performed to remove debris and bacteria from the affected area. Dressings are regularly changed to maintain a clean healing environment. Patients are monitored for signs of infection such as fever, redness, or swelling. Severe infections can lead to systemic complications such as sepsis if not treated promptly. Effective infection control is essential for successful surgical outcomes.
Pain Management in Sever Wound Surgery Patients
Pain control is an essential component of sever wound surgery care. Anesthesia is administered during surgery to ensure patient comfort and immobility. Depending on the injury, local, regional, or general anesthesia may be used. Post-surgical pain is managed using a combination of medications. Nerve blocks may be applied to target specific pain areas. Multimodal pain management strategies reduce reliance on high-dose opioids. Psychological support may also be provided to help patients cope with trauma-related stress. Effective pain management improves recovery speed and overall patient well-being.
Recovery and Healing After Sever Wound Surgery
Healing after sever wound surgery occurs in multiple biological stages. The body first focuses on clotting and stopping bleeding immediately after surgery. Inflammation follows, helping remove damaged tissue and prevent infection. New tissue formation begins as cells regenerate and repair injured areas. Scar tissue develops over time as the wound strengthens. Physical therapy is often required to restore mobility and strength. Nutrition plays a crucial role in supporting tissue regeneration and immune function. Regular follow-up appointments ensure proper healing progression and early detection of complications.
Complications Associated with Sever Wound Surgery
Despite advances in medical care, sever wound surgery may still involve complications. Infection remains one of the most common risks, especially in contaminated wounds. Excessive bleeding can occur during or after surgery, requiring further intervention. Nerve damage may result in loss of sensation or motor function. Scar tissue formation can sometimes limit movement or cause discomfort. Delayed healing is more common in patients with underlying conditions such as diabetes. Surgical graft failure may require additional procedures. Continuous monitoring helps reduce the likelihood of severe complications.
Innovations in Sever Wound Surgery
Modern advancements have significantly improved outcomes in sever wound surgery. Robotic-assisted surgical systems allow for greater precision in complex procedures. Regenerative medicine is being used to enhance tissue repair and healing. Bioengineered skin substitutes provide alternatives for patients with extensive burns or wounds. 3D printing technology is used to create customized tissue scaffolds. Smart dressings can monitor wound conditions in real time. Minimally invasive techniques reduce recovery time and surgical trauma. These innovations continue to transform trauma care and improve survival rates.
Rehabilitation and Long-Term Care After Sever Wound Surgery
Rehabilitation is essential for full recovery after sever wound surgery. Physical therapy helps restore strength, movement, and coordination. Occupational therapy assists patients in returning to daily activities and work. Psychological counseling may be needed to address emotional trauma. Long-term care includes monitoring for chronic pain or mobility issues. Adaptive devices may be required depending on injury severity. Lifestyle modifications help support long-term healing and prevent complications. Continuous rehabilitation improves independence and quality of life.
When Medical Intervention Becomes Necessary for Severe Wounds
Immediate medical attention is required when injuries clearly indicate the need for sever wound surgery. Signs such as uncontrolled bleeding, deep tissue exposure, or deformity should never be ignored. Loss of sensation or movement suggests possible nerve or spinal involvement. Visible contamination increases the risk of infection and requires urgent care. Trauma centers provide specialized treatment for complex injuries. Delayed symptoms such as persistent pain or swelling also require evaluation. Early intervention significantly improves recovery outcomes and reduces complications.
Prevention Strategies for Severe Injury Avoidance
Preventing injuries that require sever wound surgery involves proactive safety measures. Wearing protective equipment in workplaces reduces accident risks significantly. Road safety practices such as seatbelt use help prevent trauma during collisions. Sports safety equipment minimizes injury during physical activities. Home safety awareness reduces risks of falls and accidents. Workplace training programs improve hazard recognition and prevention. Public education campaigns help increase awareness of injury prevention strategies. Prevention remains the most effective approach to reducing severe trauma cases.
Frequently Asked Questions (FAQ)
What conditions require sever wound surgery?
Sever wound surgery is required for deep injuries involving muscles, nerves, blood vessels, or bones that cannot heal naturally.
How urgent is sever wound surgery?
Many cases are medical emergencies requiring immediate surgical intervention.
What is the recovery timeline?
Recovery can range from several weeks to months depending on injury severity.
Are there risks involved?
Yes, including infection, bleeding, nerve damage, and delayed healing.
Can wounds heal without surgery?
Minor injuries may heal without surgery, but most severe wounds require surgical treatment.
Will scarring occur?
Yes, but reconstructive techniques aim to minimize visible scarring.
Key Insight Section
Effective sever wound surgery depends on rapid diagnosis, precise surgical intervention, and structured rehabilitation. Early treatment dramatically improves functional recovery and reduces long-term complications.