Understanding Corneal Transplant
A corneal transplant is a specialized surgical procedure aimed at replacing a damaged or diseased cornea with healthy tissue from a donor. The cornea is the eye’s transparent outer layer, responsible for focusing light and ensuring clear vision. Damage to this critical part of the eye can result from conditions like scarring, infections, degenerative disorders, or injuries, often leading to blurred vision or even blindness. Corneal transplants are designed to restore visual clarity, reduce pain, and improve overall eye health. There are several types of transplants performed based on the extent of corneal damage. Penetrating Keratoplasty replaces the full thickness of the cornea. Endothelial Keratoplasty focuses on the inner layer, leaving the outer layers intact. Deep Anterior Lamellar Keratoplasty targets the front layers while preserving healthy tissue. Understanding these distinctions is vital for patients considering surgery, as it directly affects recovery time and long-term results.
Who Should Consider a Corneal Transplant
Patients may need a corneal transplant when traditional treatments, such as glasses, contact lenses, or medications, are insufficient. Common conditions that lead to this surgery include keratoconus, where the cornea thins and bulges, and Fuchs’ dystrophy, which gradually deteriorates the cornea’s inner layer. Other causes include corneal scarring from injuries, infections, and repeated inflammation. Risk factors may also include prior eye surgeries, chronic eye diseases, and genetic predispositions. Early symptoms can signal the need for intervention, such as distorted vision, sensitivity to light, persistent pain, or difficulty reading. Recognizing these warning signs and seeking timely evaluation can make a significant difference in surgical outcomes. Ophthalmologists assess each patient individually to determine the best type of transplant.
Preparing for Corneal Transplant Surgery
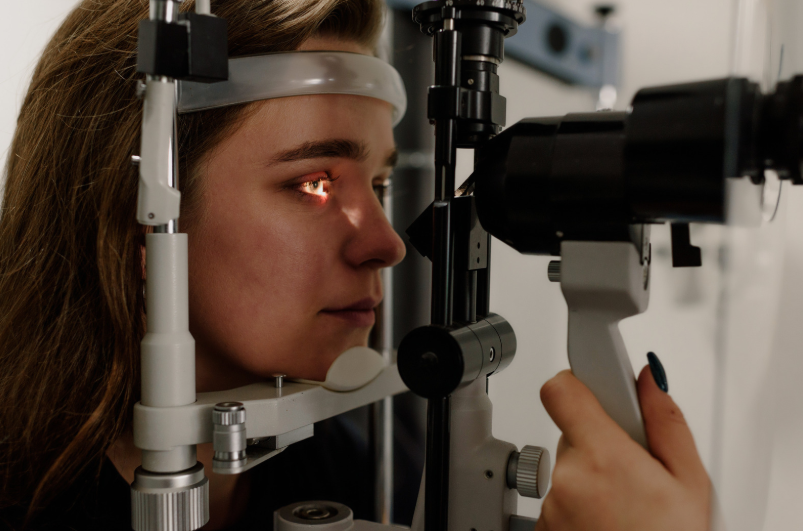
Successful corneal transplant outcomes depend on thorough preoperative preparation. Patients undergo a detailed eye examination, including tests like corneal topography, pachymetry, and endothelial cell count. These assessments evaluate the shape, thickness, and health of the cornea and surrounding structures. Patients may be asked to adjust medications, manage underlying health conditions like diabetes or hypertension, and temporarily discontinue certain eye drops. Lifestyle factors, including proper nutrition, hydration, and avoiding smoking, can influence healing. On the day of surgery, instructions regarding fasting, arrival time, and anesthesia are provided. Mental preparation is equally important, as understanding the procedure helps reduce anxiety and fosters cooperation with postoperative care. Being fully prepared lays the foundation for a smooth and successful surgery.
The Corneal Transplant Procedure
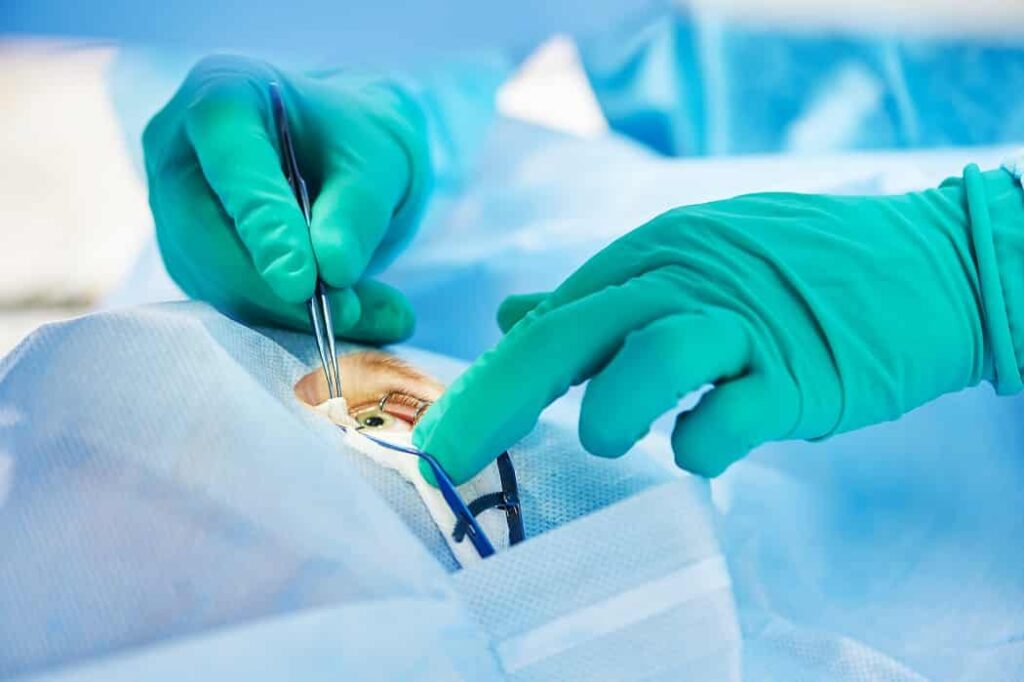
Corneal transplant surgery involves removing the damaged portion of the cornea and replacing it with healthy donor tissue. Donor corneas are carefully screened and matched to minimize the risk of rejection. The patient receives local or general anesthesia depending on individual needs and surgical complexity. The surgeon meticulously removes the affected corneal tissue and positions the donor graft with precision, securing it with fine sutures or adhesives. The surgery typically takes one to two hours, although complex cases may require longer. Modern surgical techniques and advanced instrumentation have greatly improved the safety, accuracy, and efficiency of corneal transplants. Patients generally experience minimal discomfort during the procedure, and vision restoration is often significant once healing begins. Proper surgical execution is key to long-term success.
Recovery and Rehabilitation
Recovery after a corneal transplant requires diligence and patience. In the first few days, mild discomfort, light sensitivity, and blurred vision are common. Patients are prescribed eye drops and medications to prevent infection and minimize the risk of rejection. Protective measures, such as wearing an eye shield at night and avoiding activities that could injure the eye, are essential. Regular follow-up visits with the ophthalmologist allow monitoring of healing and early detection of complications. Vision improvement is gradual, and full clarity may take several months to a year. Rehabilitation may involve corrective lenses or minor procedures to fine-tune vision. Adhering strictly to medical guidance and avoiding habits that stress the eye is critical for a successful recovery.
Potential Risks and Management Strategies
Although corneal transplants are generally safe, patients should be aware of potential complications. These may include graft rejection, infection, elevated eye pressure, and postoperative astigmatism. Signs of graft rejection include redness, discomfort, sensitivity to light, and a sudden drop in vision. Prompt medical attention and treatment with medications such as corticosteroids can often reverse rejection. Preventive strategies include proper medication use, maintaining eye hygiene, and avoiding trauma or infection. Some patients may require additional interventions to manage complications. Long-term monitoring ensures the transplanted cornea remains healthy and clear. Understanding these risks and how to address them empowers patients to take proactive steps in safeguarding vision.
Innovations in Corneal Transplantation
Advancements in corneal transplantation have improved patient outcomes and reduced recovery times. Minimally invasive techniques, like endothelial keratoplasty, allow selective replacement of the affected corneal layers while preserving healthy tissue. Artificial corneas and bioengineered tissue are emerging alternatives for patients with limited donor availability. State-of-the-art imaging and surgical tools enhance precision, reduce complications, and accelerate healing. Research into regenerative medicine holds promise for stimulating corneal cell growth, potentially reducing the need for donor tissue. These innovations make corneal transplant surgery safer, more accessible, and more effective than ever before. Staying informed about modern options allows patients to discuss the most appropriate procedure with their ophthalmologist.
Adjusting to Life After a Corneal Transplant
Living with a transplanted cornea requires careful management and attention. Vision restoration may not be immediate, and patients need to adapt to changes in depth perception, glare sensitivity, and visual sharpness. Regular ophthalmology visits, consistent use of prescribed medications, and protective eye measures are essential. Lifestyle adjustments, including limiting screen exposure and practicing good eye hygiene, support long-term outcomes. Emotional well-being is also important, as vision restoration often impacts daily routines, independence, and confidence. Connecting with support networks and educational resources can help patients navigate these changes. Following these practices ensures optimal vision and overall eye health over the years.
Frequently Asked Questions (FAQ)
- How long does a corneal transplant last?
Most corneal transplants can last 10 to 20 years, depending on individual health, age, and adherence to care instructions. - Is the procedure painful?
Patients typically experience mild discomfort, and anesthesia minimizes pain during surgery. - How soon will I notice improved vision?
Vision gradually improves over weeks to months, with full clarity often achieved within a year. - Can corneal transplants fail?
While rare, graft rejection or failure can occur, and sometimes a repeat transplant may be necessary. - What signs indicate rejection?
Redness, pain, light sensitivity, and blurred vision are warning signs that require immediate medical attention. - Are there alternatives to corneal transplantation?
Options include specialized contact lenses, corneal cross-linking, or artificial corneas for those not eligible for donor tissue.
Takeaway
Corneal transplant surgery offers a transformative path to restoring vision and improving eye health for patients with damaged or diseased corneas. With careful preparation, adherence to post-surgery care, and awareness of potential risks, patients can achieve lasting improvements in vision. Modern surgical techniques and emerging innovations make the procedure safer and more effective than ever. Those considering a corneal transplant can take proactive steps by consulting an ophthalmologist, understanding their options, and committing to post-surgery care. With the right approach, corneal transplantation provides a renewed sense of clarity, independence, and quality of life for countless patients.